There is much more desperation in this searching and enlightening history than there are remedies. Andrew Scull is a distinguished sociologist and scholar of psychiatry. He comes across as wise, sanguine and unsurprised by his findings in this survey of how American psychiatry has understood and treated the insane, distressed and traumatized from 1820 to the present. His book, however, will leave readers who are unfamiliar with the story horrified and aghast. Since my own breakdown and sectioning in early 2019 I have been working with sufferers, social workers and psychiatrists on improving the understanding and treatment of mental distress. Members of the Critical Psychiatry Network have struck me as particularly troubled by current psychiatric practice, and having read this book, I understand why.
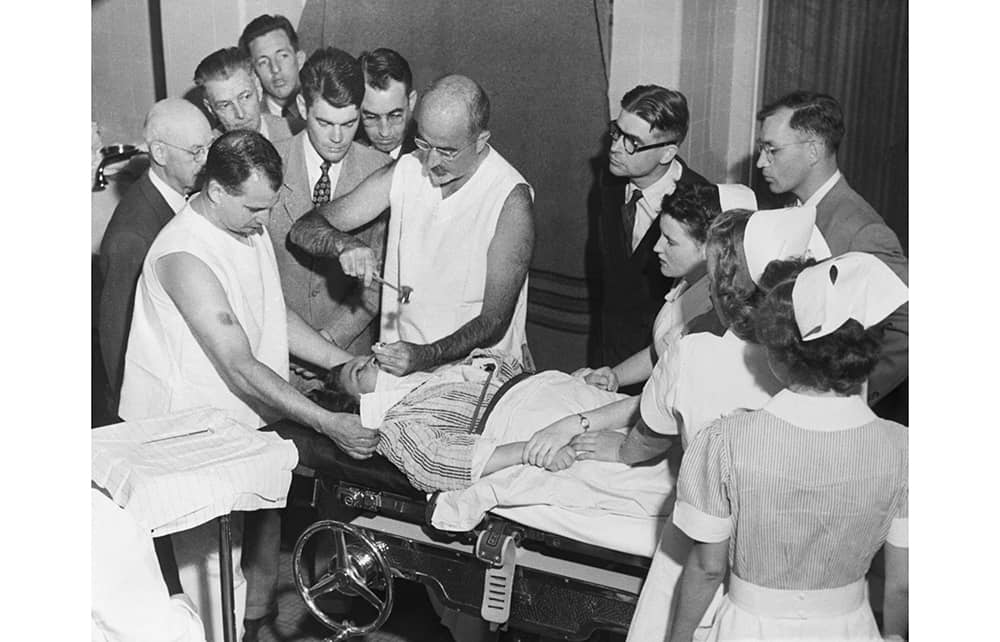
The history of psychiatry is a catalog of disastrous mistreatment. Accounts of induced comas, electric shocks, chemical straitjackets, lobotomies, brutal incarceration, injustice and cruelty on an industrial scale, and all disproportionately visited on women and black people, make appalling reading. You turn Scull’s pages waiting for something to get better. Freud and psycho-analysis provide some respite, when, for a few years, psychiatry admitted the possibility that mental distress might flow from the minds and life stories of sufferers rather than the brain, body and heredity.
But even then, psychoanalysis served the rich, while the vast majority of sufferers remained in asylums. In 1948, the journalist Albert Deutsch described them in his book The Shame of the States: “I was reminded of the pictures of the Nazi concentration camps at Belsen and Buchenwald. I entered buildings swarming with naked humans herded like cattle and treated with less concern.” He took a photographer, and psychiatrists welcomed him, because Deutsch believed the problem was not psychiatry but lack of state funding. Officials disagreed and decades of deinstitutionalization began. Mad rich people got personalized treatments, but mad poor ones, it was thought, would be better off with “care in the community.” You see them on the street corners and in the gutters of our own towns and cities.
As Scull points out, both the care and the community were and are chimeras. Thank goodness for the interventions of science and the modern psychiatrist, unswayed by Big Pharma’s lobbying, cleaving to rigorous evidence from meticulous drug trials, painstakingly and precisely dispensing the billions of dollars of psychotropic medication that millions of children, adults and the elderly now consume in response to everything from grief and anxiety to psychosis and schizophrenia. If only. In reality, American psychiatrists memorize the Diagnostic and Statistical Manual of Mental Disorders, the handbook drawn up by psychiatrists with lucrative ties to the pharmaceutical industry, which classifies people by checklists of symptoms (for some “diseases” you only need two of ten, so people suffering wildly different conditions are diagnosed with the same disorder).
Classifications correspond to treatments with drugs, the workings of which neither science nor psychiatry can explain. Prescribed by trial and error, drugs are swapped, modified or doubled up, depending on their side effects. Insurance companies pay out, pharmaceutical corporations cash in, diverting fractions of staggering profits to marketing drugs to psychiatrists, while not, notably, investing in new treatments. Universities pay influential academic psychiatrists who attract huge grants from pharmaceutical companies for trials, as long as the results are favorable to their products. The universities bank fat slices of overheads and research expenses.
The drugs do alleviate symptoms. In my experience, two doses of antipsychotics rapidly and thoroughly drained me of mania and delusions, returning to me to sanity in sixty hours after months of escalating lunacy. But they are chaotically overprescribed, wreaking storms of side effects, from weight gain to suicidal thoughts, sexual dysfunction and early death. And they are underwritten by unproven hypotheses. If you have a notion that misery and happiness depend on serotonin, and that pills might correct imbalances in the brain, well, Scull writes:
We possess no means of measuring serotonin levels in people’s brains, let alone determining what normal levels for this neurotransmitter might be. We must perforce rely on indirect evidence, and that indirect evidence fails to support the drug companies.
Where psychiatry goes now is unclear. So fragile are its foundations that Robin Murray, the former dean of the London Institute of Psychiatry, says: “I expect to see the end of the concept of schizophrenia soon. Already the evidence that it is a discrete entity rather than just the severe end of psychosis has been fatally undermined.” Psychiatry will have spent decades searching for the causes of a non-existent disease. The quest to identify genetic or physical biomarkers of mental ill health is yielding nothing. Sufferers and their families still have to endure the scourge of what is called schizophrenia, and other malign conditions.
Scull does not mention treatments such as Open Dialogue, which report near revolutionary success rates, but psychology is not his subject. I would recommend this fascinating, alarming and alerting book to anybody. For anyone referred to a psychiatrist it is surely essential.
This article was originally published in The Spectator’s UK magazine. Subscribe to the World edition here.